Understanding Bronchiectasis Treatment
Bronchiectasis is a chronic condition that affects the airways of the lungs, leading to persistent coughing, mucus production, and recurrent respiratory infections. While the condition requires long-term management, understanding the available treatment approaches and care strategies can help individuals better navigate daily life and maintain respiratory well-being.
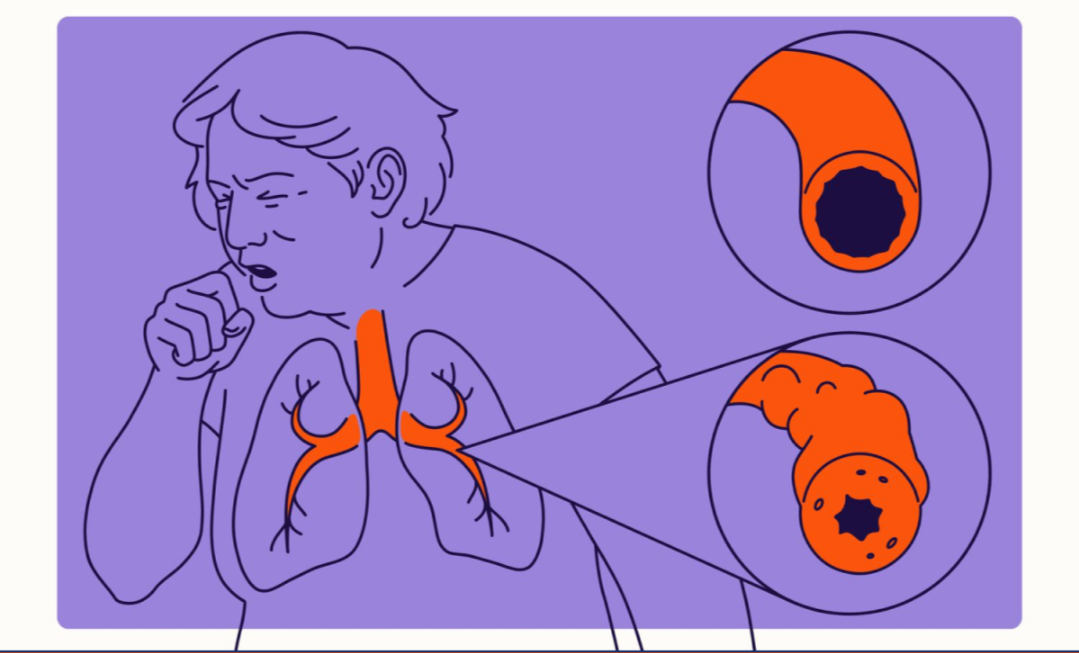
Living with a chronic respiratory condition requires understanding both the disease itself and the various ways to manage it effectively. Bronchiectasis affects thousands of Canadians, and while it cannot be cured, proper treatment can significantly improve daily functioning and reduce the frequency of complications.
What Is Bronchiectasis
Bronchiectasis is a long-term condition where the airways of the lungs become abnormally widened and damaged. This damage prevents the airways from clearing mucus properly, creating an environment where bacteria can thrive. The condition develops gradually, often following repeated lung infections, immune system problems, or inherited conditions like cystic fibrosis. Symptoms typically include a persistent cough that produces large amounts of mucus, shortness of breath, chest pain, and recurring respiratory infections. The severity varies considerably between individuals, with some experiencing mild symptoms while others face significant breathing challenges. Diagnosis usually involves imaging tests such as high-resolution CT scans, which reveal the characteristic widening of the airways. Pulmonary function tests and sputum cultures help healthcare providers assess lung capacity and identify specific bacteria present in the airways.
General Goals of Treatment
The primary objectives when managing bronchiectasis focus on preventing disease progression and maintaining respiratory health. Treatment aims to reduce the frequency and severity of lung infections, which cause further airway damage over time. Clearing mucus from the airways represents another crucial goal, as accumulated secretions provide breeding grounds for bacteria. Improving breathing capacity and reducing symptoms like coughing and shortness of breath helps patients maintain their daily activities and quality of life. Healthcare providers also work to identify and address the underlying cause of bronchiectasis when possible, though in many cases the original trigger remains unknown. Long-term management strategies emphasize preventing complications such as respiratory failure or heart problems related to chronic lung disease. Regular monitoring allows medical teams to adjust treatment plans as the condition evolves, ensuring patients receive appropriate care at each stage.
Treatment Approaches and Cost Considerations
Bronchiectasis management in Canada typically involves multiple treatment modalities, with costs varying based on severity and individual needs. Airway clearance techniques form the foundation of daily management, including chest physiotherapy, breathing exercises, and the use of devices like positive expiratory pressure systems. These devices range from simple flutter valves to more sophisticated oscillating vests, with prices varying accordingly. Medications play a significant role, including antibiotics for treating and preventing infections, bronchodilators to open airways, and mucolytics to thin mucus. Inhaled antibiotics for long-term management can be particularly costly, though many provincial drug plans provide coverage for eligible patients. Pulmonary rehabilitation programs, offered through hospitals and specialized clinics across Canada, combine exercise training, education, and breathing techniques. While coverage varies by province, many programs are accessible through referrals from respirologists or family physicians.
| Treatment Type | Provider/Method | Estimated Cost Range |
|---|---|---|
| Airway Clearance Devices | Medical supply companies | $50 - $3,000 CAD |
| Inhaled Antibiotics | Pharmacies (prescription) | $200 - $800 per month |
| Pulmonary Rehabilitation | Hospital programs | Often covered by provincial health plans |
| Chest Physiotherapy | Private clinics | $60 - $120 per session |
| Bronchodilator Inhalers | Pharmacies (prescription) | $30 - $150 per inhaler |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Medication Management Strategies
Pharmacological treatment for bronchiectasis addresses both acute infections and long-term prevention. Oral antibiotics treat active infections, with the specific medication chosen based on sputum culture results identifying the bacteria involved. Some patients with frequent infections benefit from long-term antibiotic therapy, either in oral or inhaled form, to suppress bacterial growth and reduce exacerbation frequency. Bronchodilators help relax airway muscles, making breathing easier and facilitating mucus clearance. Mucolytic agents thin respiratory secretions, making them easier to cough up during airway clearance sessions. Anti-inflammatory medications may be prescribed in certain cases, though their role in bronchiectasis treatment continues to be studied. Vaccination against influenza and pneumococcal disease represents an important preventive measure, as these infections can trigger serious complications in people with damaged airways. Healthcare providers carefully balance the benefits and potential side effects of each medication, tailoring treatment plans to individual patient needs and response patterns.
Airway Clearance and Physical Therapy
Regular airway clearance represents perhaps the most important daily activity for people with bronchiectasis. Various techniques help mobilize and remove mucus from the lungs, preventing bacterial colonization and reducing infection risk. Postural drainage uses gravity to help mucus drain from different lung segments, with patients positioning themselves in specific ways while performing breathing exercises. Active cycle of breathing techniques combine breathing control, deep breathing, and huffing to clear secretions effectively. Oscillating devices create vibrations that loosen mucus from airway walls, making it easier to expectorate. Many patients work with respiratory therapists who teach proper techniques and recommend appropriate devices based on individual needs and abilities. Consistency matters more than the specific method chosen, as regular daily clearance prevents mucus accumulation regardless of the technique used. Physical exercise also contributes to airway clearance while improving overall fitness and lung function, making activities like walking, swimming, or cycling valuable components of comprehensive management.
Monitoring and Long-Term Care
Ongoing medical supervision ensures treatment effectiveness and allows early intervention when problems arise. Regular appointments with respirologists or pulmonologists typically occur every three to six months for stable patients, with more frequent visits during periods of increased symptoms. Pulmonary function testing tracks changes in lung capacity over time, helping healthcare teams assess disease progression and treatment response. Sputum cultures performed periodically identify bacteria present in the airways, guiding antibiotic selection when infections occur. Patients learn to recognize signs of exacerbations, including increased mucus production, changes in mucus color or consistency, worsening breathlessness, or fever. Early treatment of exacerbations prevents more serious complications and reduces the risk of further airway damage. Nutritional support becomes important for some patients, as chronic respiratory conditions increase caloric needs while breathing difficulties may reduce appetite. Maintaining adequate hydration helps keep mucus thin and easier to clear, making proper fluid intake a simple but effective management strategy.
Managing bronchiectasis requires commitment to daily treatment routines and regular medical follow-up. While the condition presents ongoing challenges, appropriate treatment allows many people to maintain active, fulfilling lives. Working closely with healthcare providers, staying consistent with airway clearance techniques, and promptly addressing infections helps minimize disease progression and preserve lung function over time.